As a collective group, our mission is to preserve the fundamentals of exceptional patient care.

Meaningful Care
Our team of board-certified dermatologists, nurse practitioners, physician assistants, and aesthetic professionals are dedicated to providing the highest quality care.
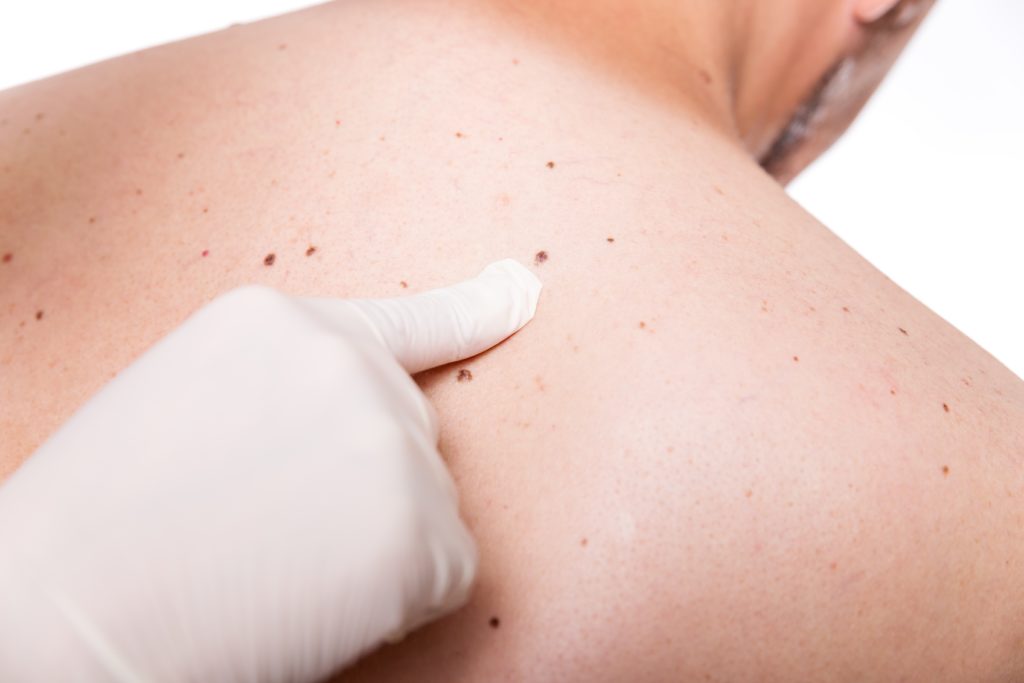
Our Services
We offer the best in medical, surgical, and cosmetic dermatology and treat everything from acute to chronic skin conditions for patients of all ages.